Can Cortisone Alleviate Hammer Toe Pain
A hammertoes occurs when the middle of the toe points upwards abnormally. This most often occurs in the second toe, and is often the result of a big toe bunion pushing on the second toe. A painful callous often forms on top of the first joint in the toe. Treatment of a hammer toe may consist of simple padding of the callous on top of the toe, as well as buying appropriate footwear. The best shoes for patients with a hammer toe will have a wide toebox, no pressure on the end of the toe, and will not press on a bunion (which may cause worsening of the hammer toe).
Causes
Medical problems, such as stroke or diabetes that affect the nerves, may also lead to hammertoe. For example, diabetes can result in poor circulation, especially in the feet. As a result, the person may not feel that their toes are bent into unnatural positions. The likelihood of developing hammertoe increases with age and may be affected by gender (more common in women) and toe length; for example, when the second toe is longer than the big toe, hammertoe is more likely to occur. Hammertoe may also be present at birth. Genetics may factor in to developing hammertoe, particularly if the foot is flat or has a high arch, resulting in instability.
 Symptoms
Symptoms
Here is a look at some of the symptoms hammertoe can cause. They include hammer-like or claw-like appearance of the toe. Pain when walking or moving the foot. Difficulty moving the toe. Corns may form on top of the toe. Callus may form on the sole of the foot. During the initial stages, you may be able to manually straighten your toe. This is called a flexible hammertoe. But as time passes, the toe will not move as easily and will continue to look like a hammer. Pressure and irritation over the joint can cause a blister to develop and become a corn over time. These corns have the potential to become infected and cause additional symptoms such as redness, bleeding, and difficulty wearing shoes and socks. Corns are the main cause of pain when hammertoes are developing.
Diagnosis
Hammer toes may be easily detected through observation. The malformation of the person's toes begin as mild distortions, yet may worsen over time - especially if the factors causing the hammer toes are not eased or removed. If the condition is paid attention to early enough, the person's toes may not be permanently damaged and may be treated without having to receive surgical intervention. If the person's toes remain untreated for too long, however the muscles within the toes might stiffen even more and will require invasive procedures to correct the deformity.
Non Surgical Treatment
Treatment options for a hammertoe are based on the severity of the condition. A hammertoe caused by inappropriate footwear can be corrected by wearing properly fitting shoes. If Hammer toe a high arch caused the condition, wearing toe pads or insoles in your shoes can help. These pads work by shifting your toe?s position, which relieves pain and corrects the appearance of your toe.
Surgical Treatment
Ordinary hammertoe procedures often use exposed wires which extend outside the end of toes for 4-6 weeks. Common problems associated with wires include infection where the wires come out of the toe, breakage, pain from hitting the wire, and lack of rotational stability causing the toe to look crooked. In addition, wires require a second in-office procedure to remove them, which can cause a lot of anxiety for many patients. Once inserted, implants remain within the bone, correcting the pain and deformity of hammertoes while eliminating many of the complications specific traditional treatments.
 Prevention
Prevention
Although the feet naturally change over time, and abnormalities like hammertoes may be hereditary for some patients, steps may be taken to prevent their development in the first place. Just as better fitting shoes are a treatment, they are also a preventative measure for hammertoes. In addition, your podiatrist may suggest orthotics to improve the biomechanics of your feet in an effort to prevent the development of hammertoes or other abnormalities. Calf stretching and other exercises may also be used to reverse or treat muscle imbalances that could eventually lead to hammertoe development.
How To Treat Tailor'S Bunion Without Surgery
Overview
 A bunion or hallux abducto valgus occurs when your big toe points toward your second toe. The big toe will touch the second or causes the second toe to overlap the big toe. This causes a boney bump to appear on the outside edge of your big toe. Bunions are more common in women and can sometimes run in families. Hallux abducto valgus can develop as a result of an inherited structural defect or stress on your foot or due to a medical condition such as arthritis. If there is an underlying structural defect in your foot this can lead to compensations causing stresses and pressures to be applied unevenly on the joints and tendons in your feet. This imbalance in pressure and stress makes your big toe joint unstable. Over time this causes the medial side of the 1st metatarsal head to develop excess bone that protrudes out beyond the normal shape of your foot. The size of the bunion can get larger over time which causes further crowding your other toes and causing pain. Pain from a bunion can be severe enough to keep you from walking comfortably in normal shoes. The condition may become painful as the bump gets worse, and extra bone and a fluid-filled sac (bursa) grow at the base of the big toe. By pushing your big toe inward, a bunion can squeeze your other toes into abnormal positions. This crowding can cause the four smaller toes to become bent or a claw-like in shape. These bent toes are known as hammertoes. Smaller bunions called ?bunionettes? can also develop on the joint of your 5th toe.
A bunion or hallux abducto valgus occurs when your big toe points toward your second toe. The big toe will touch the second or causes the second toe to overlap the big toe. This causes a boney bump to appear on the outside edge of your big toe. Bunions are more common in women and can sometimes run in families. Hallux abducto valgus can develop as a result of an inherited structural defect or stress on your foot or due to a medical condition such as arthritis. If there is an underlying structural defect in your foot this can lead to compensations causing stresses and pressures to be applied unevenly on the joints and tendons in your feet. This imbalance in pressure and stress makes your big toe joint unstable. Over time this causes the medial side of the 1st metatarsal head to develop excess bone that protrudes out beyond the normal shape of your foot. The size of the bunion can get larger over time which causes further crowding your other toes and causing pain. Pain from a bunion can be severe enough to keep you from walking comfortably in normal shoes. The condition may become painful as the bump gets worse, and extra bone and a fluid-filled sac (bursa) grow at the base of the big toe. By pushing your big toe inward, a bunion can squeeze your other toes into abnormal positions. This crowding can cause the four smaller toes to become bent or a claw-like in shape. These bent toes are known as hammertoes. Smaller bunions called ?bunionettes? can also develop on the joint of your 5th toe.
Causes
Causes of bunions are foot injuries, neuromuscular disorders, or congenital deformities. People who suffer from flat feet or low arches are also prone to developing these problems, as are arthritic patients and those with inflammatory joint disease. Occupations that place undue stress on the feet are also a factor; ballet dancers, for instance, often develop the condition. Wearing shoes that are too tight or cause the toes to be squeezed together is also a common factor, one that explains the high prevalence of the disorder among women.
Symptoms
The symptoms of hallux valgus usually center on the bunion. The bunion is painful. The severe hallux valgus deformity is also distressing to many and becomes a cosmetic problem. Finding appropriate shoe wear can become difficult, especially for women who want to be fashionable but have difficulty tolerating fashionable shoe wear. Finally, increasing deformity begins to displace the second toe upward and may create a situation where the second toe is constantly rubbing on the shoe.
Diagnosis
Diagnosis begins with a careful history and physical examination by your doctor. This will usually include a discussion about shoe wear and the importance of shoes in the development and treatment of the condition. X-rays will probably be suggested. This allows your doctor to measure several important angles made by the bones of the feet to help determine the appropriate treatment.
Non Surgical Treatment
Patients who suffer from bunions are usually referred to a surgeon. Unfortunately, surgery often makes the problem worse. Surgeons will use x-ray technology as a diagnostic tool, which does not always properly diagnose the pain source. Another problem with this approach is that it does not do anything to strengthen the weakened ligament in the foot and, thus, does not alleviate the chronic pain that people with this condition experience. Another standard practice of modern medicine is to use steroids or to prescribe anti-inflammatory medications. However, in the long run, these treatments do more damage than good. Cortisone shots and anti-inflammatory drugs have been shown to produce short-term pain benefit, but both result in long-term loss of function and even more chronic pain by actually inhibiting the healing process of soft tissues and accelerating cartilage degeneration. Plus, long-term use of these drugs can lead to other sources of chronic pain, allergies and leaky gut syndrome.
Surgical Treatment
Sometimes a screw is placed in the foot to hold a bone in a corrected position, other times a pin, wire or plate is chosen. There are even absorbable pins and screws, which are used for some patients. In British Columbia, pins seem to be used most frequently, as they're easier to insert and less expensive. They are typically--but not always--removed at some point in the healing process. But as a general rule, Dr. Schumacher prefers to use screws whenever possible, as they offer some advantages over pins. First, using screws allows you to close over the wound completely, without leaving a pin sticking out of the foot. That allows for a lower infection rate, it allows you to get your foot wet more quickly following the surgery, and it usually allows for a quicker return to normal shoes. Second, they're more stable than pins and wires. Stability allows for faster, more uneventful, bone healing. Third, they usually don't need to be removed down the road, so there's one less procedure involved.
Prevention
Because bunions develop slowly, taking care of your feet during childhood and early adulthood can pay off later in life. Keep track of the shape of your feet as they develop over time, especially if foot problems run in your family. Exercising your feet can strengthen them. Learn to pick up small objects, like a pencil or pebble, with your toes. Wear shoes that fit properly and don't cramp or pinch your toes. Women should avoid shoes with very high heels or pointed toes.
The Truth About Overpronation Of The Feet
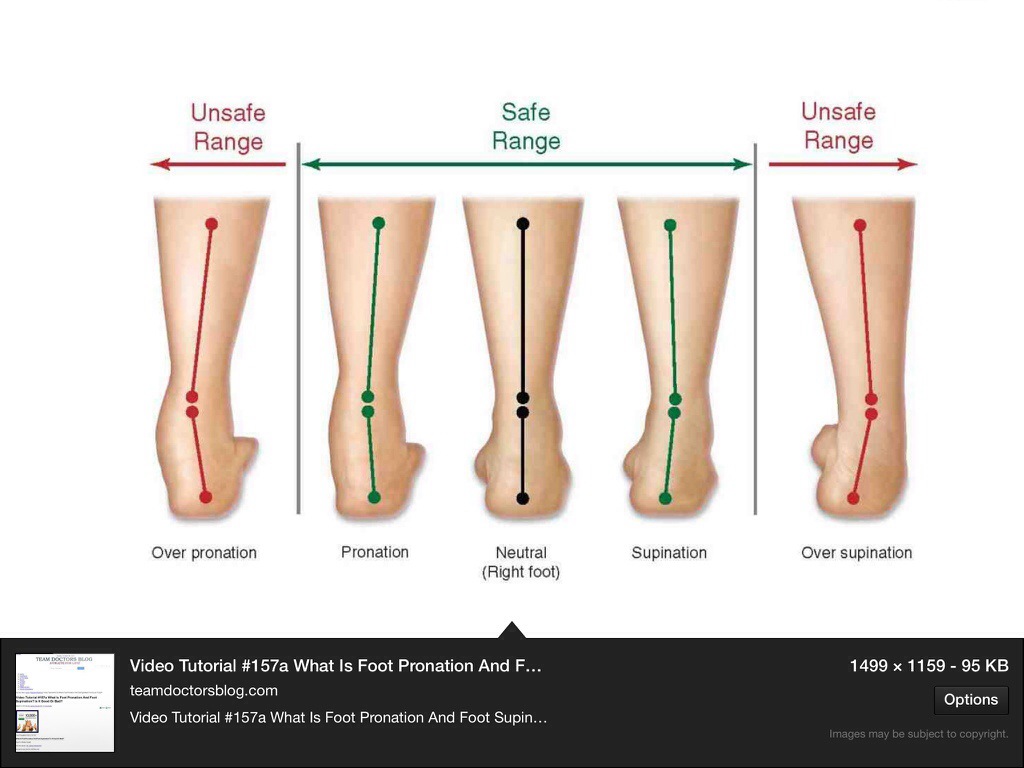
Over-pronation, or flat feet, is a common biomechanical problem that occurs in the walking process when a person?s arch collapses upon weight bearing. This motion can cause extreme stress or inflammation on the plantar fascia, possibly causing severe discomfort and leading to other foot problems.

Causes
Congenital "Flat Feet" - an individual may be born with feet that lack an appropriately supportive arch thereby predisposing the individual to this foot condition. Excessive Weight (Obesity) Too much weight on the foot from either obesity or pregnancy may be a factor. Repetitive Impact walking on flat, hard surfaces continuously places unnatural stress on the foot arch.
Symptoms
Symptoms can manifest in many different ways. The associated conditions depend on the individual lifestyle of each patient. Here is a list of some of the conditions associated with over Pronation. Hallux Abducto Valgus (bunions). Hallux Rigidus (stiff 1st toe). Arch Pain. Heel Pain (plantar Facsitus). Metatarsalgia (ball of the foot pain). Ankle Sprains. Shin Splints. Achilles Tendonitis. Osteochondrosis. Knee Pain. Corns & Calluses. Flat Feet. Hammer Toes.
Diagnosis
Your healthcare provider will ask about your symptoms, medical history, and activities and examine your feet. Your provider may watch you walk or run. Check the motion of your feet when they strike the ground. Look at your athletic shoes to see if they show an abnormal pattern of wear.
Non Surgical Treatment
No matter what the cause in your case, over pronation can be remedied in several ways. Those who are overweight should consider permanently losing weight to naturally alleviate pressure on the ligaments and heel of the foot. Also, you should consult a podiatrist to examine your posture and movement habits. You may be reinjuring yourself due to poor alignment without even knowing it. If you also have lower back problems, this could be a sign of over pronation as a result of misalignment.
Prevention
Wear supportive shoes. If we're talking runners you're going to fall in the camp of needing 'motion control' shoes or shoes built for 'moderate' or 'severe' pronators. There are many good brands of shoes out there. Don't just wear these running, the more often the better. Make slow changes. Sudden changes in your training will aggravate your feet more than typical. Make sure you slowly increase your running/walking distance, speed and even how often you go per week. Strengthen your feet. As part of your running/walking warm up or just as part of a nightly routine try a few simple exercises to strengthen your feet, start with just ten of each and slowly add more sets and intensity. Stand facing a mirror and practice raising your arch higher off the ground without lifting your toes. Sit with a towel under your feet, scrunch your toes and try to pull the towel in under your feet. Sitting again with feet on the ground lift your heels as high as you can, then raise and lower on to toe tips.
Treating Severs Disease
If you?re a young basketballer/netballer/footballer and have heel pain when playing basketball or sports involving running or jumping, you may have a particular growth pain disorder called Sever?s Disease. It is a condition (not a disease) usually affecting 9-15 year olds that occurs at the back of the heel, where the Achilles tendon attaches to the foot. The Achilles tendon is the tendon connected to the calf muscles. Pulling of the calf muscles results in tension in the Achilles and in adolescents, repeated running/jumping can result in pain and inflammation at the heel, this is called Sever?s Disease.
Causes
Overuse and stress on the heel bone through participation in sports is a major cause of calcaneal apophysitis. The heel?s growth plate is sensitive to repeated running and pounding on hard surfaces, resulting in muscle strain and inflamed tissue. For this reason, children and adolescents involved in soccer, track, or basketball are especially vulnerable. Other potential causes of calcaneal apophysitis include obesity, a tight Achilles tendon, and biomechanical problems such as flatfoot or a high-arched foot.
Symptoms
Symptoms of Sever?s disease, mostly pain at the back of heel, usually occur during and after sporting activity, and usually disappear with rest. In some cases, children may find it difficult to place pressure on their heels, and begin walking on their toes to gain relief. For some children, the heel pain will persist until the next morning, causing some stiffness or hobbling on first arising. Some children may experience mild swelling at the back of the heel.
Diagnosis
In Sever's disease, heel pain can be in one or both heels. It usually starts after a child begins a new sports season or a new sport. Your child may walk with a limp. The pain may increase when he or she runs or jumps. He or she may have a tendency to tiptoe. Your child's heel may hurt if you squeeze both sides toward the very back. This is called the squeeze test. Your doctor may also find that your child's heel tendons have become tight.
Non Surgical Treatment
The physiotherapist will thoroughly assess the affected areas and general mechanics to determine what factors may be contributing, also to rule out any other injuries or stress fractures, etc. Treatment focusing on the affected area will consist of modified rest, ice, massage, stretches and electrotherapy. A foam heel raise may also be given to help decrease pain. The physiotherapist may also treat other areas if biomechanical problems are noted. This may include massage, mobilization and exercises to stretch and strengthen certain areas. They may also refer the patient to see a podiatrist if they believe the foot posture is a factor.
Exercise
Exercises that help to stretch the calf muscles and hamstrings are effective at treating Sever's disease. An exercise known as foot curling, in which the foot is pointed away from the body, then curled toward the body in order to help stretch the muscles, has also proven to be very effective at treating Sever's disease. The curling exercise should be done in sets of 10 or 20 repetitions, and repeated several times throughout the day.
What Exactly Is Adult Aquired Flat Foot ?
Overview
Posterior tibial tendon insufficiency (also called posterior tibial tendon dysfunction or adult acquired flatfoot) has been named literally after failure of the posterior tibial tendon. However, the condition is caused not only by the progressive failure of the posterior tibial tendon; it is also failure of associated ligaments and joints on the inner side of the ankle and foot. This results in collapse of the arch of the foot, along with the deformity which most often becomes the debilitating problem in its later stages. While at the beginning the common symptom is pain over the tendon in the inner part of the hindfoot and midfoot, later on it is the deformity that can threaten a person?s ability to walk. Just as the tendon degenerates and loses its function, other soft tissue on the same inner side of the foot - namely the ligaments - degenerate and fail. Ligaments are responsible for holding bones in place, and when they fail, bones shift to places where they shouldn?t; deformity is the result. The deformity causes malalignment, leading to more stress and failure of the ligaments. 
Causes
Overuse of the posterior tibial tendon is often the cause of PTTD. In fact, the symptoms usually occur after activities that involve the tendon, such as running, walking, hiking, or climbing stairs.
Symptoms
Most people will notice mild to extreme pain in their feet. Below outlines some signs and symptoms of AAFD. Trouble walking or standing for any duration. Pain and swelling on the inside of the ankle. Bump on the bottom of the foot. Ulcer or wound developing on the outer aspects of foot.
Diagnosis
In the early stages of dysfunction of the posterior tibial tendon, most of the discomfort is located medially along the course of the tendon and the patient reports fatigue and aching on the plantar-medial aspect of the foot and ankle. Swelling is common if the dysfunction is associated with tenosynovitis. As dysfunction of the tendon progresses, maximum pain occurs laterally in the sinus tarsi because of impingement of the fibula against the calcaneus. With increasing deformity, patients report that the shape of the foot changes and that it becomes increasingly difficult to wear shoes. Many patients no longer report pain in the medial part of the foot and ankle after a complete rupture of the posterior tibial tendon has occurred; instead, the pain is located laterally. If a fixed deformity has not occurred, the patient may report that standing or walking with the hindfoot slightly inverted alleviates the lateral impingement and relieves the pain in the lateral part of the foot.
Non surgical Treatment
The following is a summary of conservative treatments for acquired flatfoot. Stage 1, NSAIDs and short-leg walking cast or walker boot for 6-8 weeks; full-length semirigid custom molded orthosis, physical therapy. Stage 2, UCBL orthosis or short articulated ankle orthosis. Stage 3, Molded AFO, double-upright brace, or patellar tendon-bearing brace. Stage 4, Molded AFO, double-upright brace, or patellar tendon-bearing brace. 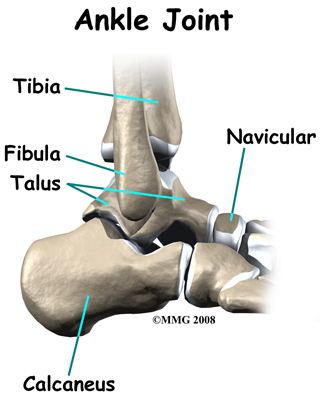
Surgical Treatment
Surgery should only be done if the pain does not get better after a few months of conservative treatment. The type of surgery depends on the stage of the PTTD disease. It it also dictated by where tendonitis is located and how much the tendon is damaged. Surgical reconstruction can be extremely complex. Some of the common surgeries include. Tenosynovectomy, removing the inflamed tendon sheath around the PTT. Tendon Transfer, to augment the function of the diseased posterior tibial tendon with a neighbouring tendon. Calcaneo-osteotomy, sometimes the heel bone needs to be corrected to get a better heel bone alignment. Fusion of the Joints, if osteoarthritis of the foot has set in, fusion of the joints may be necessary.
What Is The Cause And Treatment Of Posterior Tibial Tendon Dysfunction
Overview Tendons do a lot of work. In fact, a great deal of what happens when you walk can be related to tendons tugging and pulling in appropriate ways in their proper places. With this in mind, it?s hardly surprising that on occasion, (probably because we too often forget to send them ?Thank you? cards), tendons may decide that they?ve had it. They may buck their responsibilities, shirk their work, and in all other ways cease to function properly. And that may mean bad news for you. Take the posterior tibial tendon: it runs from the bottom of the calf, goes right under that bump on the inside of the ankle (the medial malleolus) and ends up attaching itself to a bone on the inside of the middle of your foot (the navicular bone). It?s the main tendon that keeps the arch of your foot in place, and it helps a bunch in walking, too. Over time, though, we tend to put a lot of stress on this faithful tendon, especially if we?ve put on extra weight, or do a lot of activities that stress it out, walking, running, hiking, or climbing stairs. Sometimes athletes (who do a lot of that walking and running stuff) may put so much stress on the tendon that it tears suddenly. But for many of us, damage may take place gradually (i.e. the tendon stretches out) until the tendon tells us that it flat out quits. (It sometimes doesn?t even give two weeks notice.) In short, you may develop posterior tibial tendon dysfunction (PTTD).  Causes There are numerous causes of acquired adult flatfoot, including fracture or dislocation, tendon laceration, tarsal coalition, arthritis, neuroarthropathy, neurologic weakness, and iatrogenic causes. The most common cause of acquired adult flatfoot is posterior tibial tendon dysfunction. Symptoms Your feet tire easily or become painful with prolonged standing. It's difficult to move your heel or midfoot around, or to stand on your toes. Your foot aches, particularly in the heel or arch area, with swelling along the inner side. Pain in your feet reduces your ability to participate in sports. You've been diagnosed with rheumatoid arthritis; about half of all people with rheumatoid arthritis will develop a progressive flatfoot deformity. Diagnosis It is of great importance to have a full evaluation, by a foot and ankle specialist with expertise in addressing complex flatfoot deformities. No two flat feet are alike; therefore, "Universal" treatment plans do not exist for the Adult Flatfoot. It is important to have a custom treatment plan that is tailored to your specific foot. That starts by first understanding all the intricacies of your foot, through an extensive evaluation. X-rays of the foot and ankle are standard, and MRI may be used to better assess the quality of the PT Tendon. Non surgical Treatment PTTD is a progressive condition. Early treatment is needed to prevent relentless progression to a more advanced disease which can lead to more problems for that affected foot. In general, the treatments include rest. Reducing or even stopping activities that worsen the pain is the initial step. Switching to low-impact exercise such as cycling, elliptical trainers, or swimming is helpful. These activities do not put a large impact load on the foot. Ice. Apply cold packs on the most painful area of the posterior tibial tendon frequently to keep down the swelling. Placing ice over the tendon immediately after completing an exercise helps to decrease the inflammation around the tendon. Nonsteroidal Anti-inflammatory Medication (NSAIDS). Drugs, such as arcoxia, voltaren and celebrex help to reduce pain and inflammation. Taking such medications prior to an exercise activity helps to limit inflammation around the tendon. However, long term use of these drugs can be harmful to you with side effects including peptic ulcer disease and renal impairment or failure. Casting. A short leg cast or walking boot may be used for 6 to 8 weeks in the acutely painful foot. This allows the tendon to rest and the swelling to go down. However, a cast causes the other muscles of the leg to atrophy (decrease in strength) and thus is only used if no other conservative treatment works. Most people can be helped with orthotics and braces. An orthotic is a shoe insert. It is the most common non-surgical treatment for a flatfoot and it is very safe to use. A custom orthotic is required in patients who have moderate to severe changes in the shape of the foot. Physiotherapy helps to strengthen the injured tendon and it can help patients with mild to moderate disease of the posterior tibial tendon.
Causes There are numerous causes of acquired adult flatfoot, including fracture or dislocation, tendon laceration, tarsal coalition, arthritis, neuroarthropathy, neurologic weakness, and iatrogenic causes. The most common cause of acquired adult flatfoot is posterior tibial tendon dysfunction. Symptoms Your feet tire easily or become painful with prolonged standing. It's difficult to move your heel or midfoot around, or to stand on your toes. Your foot aches, particularly in the heel or arch area, with swelling along the inner side. Pain in your feet reduces your ability to participate in sports. You've been diagnosed with rheumatoid arthritis; about half of all people with rheumatoid arthritis will develop a progressive flatfoot deformity. Diagnosis It is of great importance to have a full evaluation, by a foot and ankle specialist with expertise in addressing complex flatfoot deformities. No two flat feet are alike; therefore, "Universal" treatment plans do not exist for the Adult Flatfoot. It is important to have a custom treatment plan that is tailored to your specific foot. That starts by first understanding all the intricacies of your foot, through an extensive evaluation. X-rays of the foot and ankle are standard, and MRI may be used to better assess the quality of the PT Tendon. Non surgical Treatment PTTD is a progressive condition. Early treatment is needed to prevent relentless progression to a more advanced disease which can lead to more problems for that affected foot. In general, the treatments include rest. Reducing or even stopping activities that worsen the pain is the initial step. Switching to low-impact exercise such as cycling, elliptical trainers, or swimming is helpful. These activities do not put a large impact load on the foot. Ice. Apply cold packs on the most painful area of the posterior tibial tendon frequently to keep down the swelling. Placing ice over the tendon immediately after completing an exercise helps to decrease the inflammation around the tendon. Nonsteroidal Anti-inflammatory Medication (NSAIDS). Drugs, such as arcoxia, voltaren and celebrex help to reduce pain and inflammation. Taking such medications prior to an exercise activity helps to limit inflammation around the tendon. However, long term use of these drugs can be harmful to you with side effects including peptic ulcer disease and renal impairment or failure. Casting. A short leg cast or walking boot may be used for 6 to 8 weeks in the acutely painful foot. This allows the tendon to rest and the swelling to go down. However, a cast causes the other muscles of the leg to atrophy (decrease in strength) and thus is only used if no other conservative treatment works. Most people can be helped with orthotics and braces. An orthotic is a shoe insert. It is the most common non-surgical treatment for a flatfoot and it is very safe to use. A custom orthotic is required in patients who have moderate to severe changes in the shape of the foot. Physiotherapy helps to strengthen the injured tendon and it can help patients with mild to moderate disease of the posterior tibial tendon.  Surgical Treatment In cases of PTTD that have progressed substantially or have failed to improve with non-surgical treatment, surgery may be required. For some advanced cases, surgery may be the only option. Surgical treatment may include repairing the tendon, tendon transfers, realigning the bones of the foot, joint fusions, or both. Dr. Piccarelli will determine the best approach for your specific case. A variety of surgical techniques is available to correct flexible flatfoot. Your case may require one procedure or a combination of procedures. All of these surgical techniques are aimed at relieving the symptoms and improving foot function. Among these procedures are tendon transfers or tendon lengthening procedures, realignment of one or more bones, or insertion of implant devices. Whether you have flexible flatfoot or PTTD, to select the procedure or combination of procedures for your particular case, Dr. Piccarelli will take into consideration the extent of your deformity based on the x-ray findings, your age, your activity level, and other factors. The length of the recovery period will vary, depending on the procedure or procedures performed.
Surgical Treatment In cases of PTTD that have progressed substantially or have failed to improve with non-surgical treatment, surgery may be required. For some advanced cases, surgery may be the only option. Surgical treatment may include repairing the tendon, tendon transfers, realigning the bones of the foot, joint fusions, or both. Dr. Piccarelli will determine the best approach for your specific case. A variety of surgical techniques is available to correct flexible flatfoot. Your case may require one procedure or a combination of procedures. All of these surgical techniques are aimed at relieving the symptoms and improving foot function. Among these procedures are tendon transfers or tendon lengthening procedures, realignment of one or more bones, or insertion of implant devices. Whether you have flexible flatfoot or PTTD, to select the procedure or combination of procedures for your particular case, Dr. Piccarelli will take into consideration the extent of your deformity based on the x-ray findings, your age, your activity level, and other factors. The length of the recovery period will vary, depending on the procedure or procedures performed.